
4 Physiotherapy Tips for Osteoarthritis
Osteoarthritis is the most common form of arthritis, and although it is often related to aging
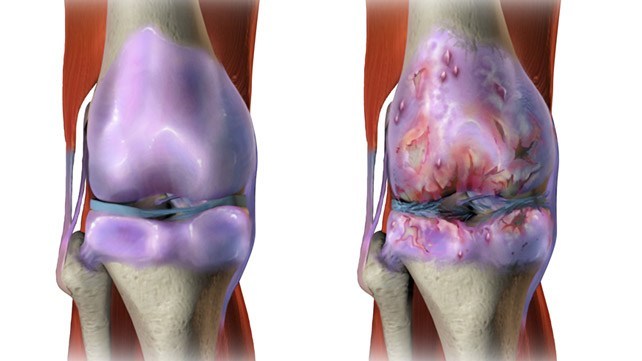
Osteoarthritis is the most common type of arthritis. According to the National Health Service, UK, approximately 8.5 million people are affected by the condition.
Osteoarthritis is a progressive disease; signs and symptoms gradually worsen over time. There is no cure. However, available therapies may help with pain and swelling (inflammation), as well as keeping the patient mobile and active. Experts say that patients who take steps to actively manage their osteoarthritis are more likely to gain control over their symptoms.
The application of the ALMAG-01 device proved to be very effective in this case and this device is used in the disease prevention and maintaining a healthy lifestyle.
Any joint in the body may be affected. However, osteoarthritis is most likely to affects the patient’s:
Osteoarthritis is more common among females than males, especially after the age of 50 years. Most commonly, it develops in people aged over 40. Younger people may also be affected; usually after an injury or as a result of another joint condition.
Some people say that osteoarthritis is an inevitable part of ageing. This is untrue. There are people well into their nineties who have no clinical or functional signs of the disease.
A symptom is something the patient feels and reports, while a sign is something other people, such as the doctor detect. For example, pain may be a symptom while a rash may be a sign.
Osteoarthritis has as its main symptoms:
In some cases people with osteoarthritis may have no symptoms. Symptoms are usually only felt in either one joint, or a just a few at any one time. In many cases the symptoms come on slowly.
The knees, hips or hands are most commonly affected.
In most cases both knees are affected, unless the osteoarthritis was caused by an injury (or another condition). The patient will experience pain when walking, especially uphill or upstairs. Knees may lock into position, making it much harder to straighten the leg. The knee may make a soft, grating sound when used.
Anything that requires movement of the hip joint causes problems, such as getting in/out of a car, or putting on one’s shoes and socks.
Although pain in the hip is common, some patients with osteoarthritis in the hips experience pain in their knee (and not their hip). Less commonly, pain may be felt in the thighs, ankles and buttocks.
Typically, pain is felt whilst walking. But some people are in pain even when resting.
Three areas may be affected:
Fingers may be stiff, swollen and painful. Sometimes bumps may develop on the finger joints. In some cases, finger pain decreases and eventually goes away, while the swelling and bumps remain.
At the affected joints the fingers may bend slightly sideways. Fluid-filled lumps may develop on the backs of the fingers; they are often painful.
A bump may develop where the base of the thumb joins the wrist. This may make writing, turning keys and opening jar-tops difficult and painful.
People who have joint stiffness and swelling that persist for more than a couple of weeks, they should see their doctor. Those already on osteoarthritis medications should contact a health care professional if they experience nausea, constipation, drowsiness, abdominal discomfort, or have black/tarry stools
People suffering from osteoarthritis must do regular remedial exercises. No doubt, in remission stage bike or swimming exercise is the best. However, if you are in the acute stages of the disease, there is no substitute for remedial exercises.
The exercises improve your mobility and keep your muscles strong. Stretches help to reduce the spasm. Commonly, lumbar and cervical portions of the spine are the most affected areas, less frequently it occurs with the thoracic spine. Often enough, osteoarthritis is complicated with neurological conditions as a result of nerve ending pressing.
In the acute stage remedial exercises are performed only when pain is significantly reduced. If during the exercises pain becomes stronger, do not proceed.
CERVICAL AREA CHRONIC STAGE

Osteoarthritis is the most common form of arthritis, and although it is often related to aging
Medical Referral | Accident Attorney Referrals
Filter out the noise and nurture your inbox with health and wellness advice that’s inclusive and rooted in medical expertise.
MedicalReferral.com does not provide medical advice, diagnosis, or treatment.